16 results
Identifying the relationship between hospital rurality and antibiotic overuse
- Hannah Hardin, Valerie Vaughn, Andrea White, Jennifer Horowitz, Elizabeth McLaughlin, Julia Szymczak, Lindsay Petty, Anurag Malani, Scott Flanders, Tejal Gandhi
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s34-s35
-
- Article
-
- You have access Access
- Open access
- Export citation
-
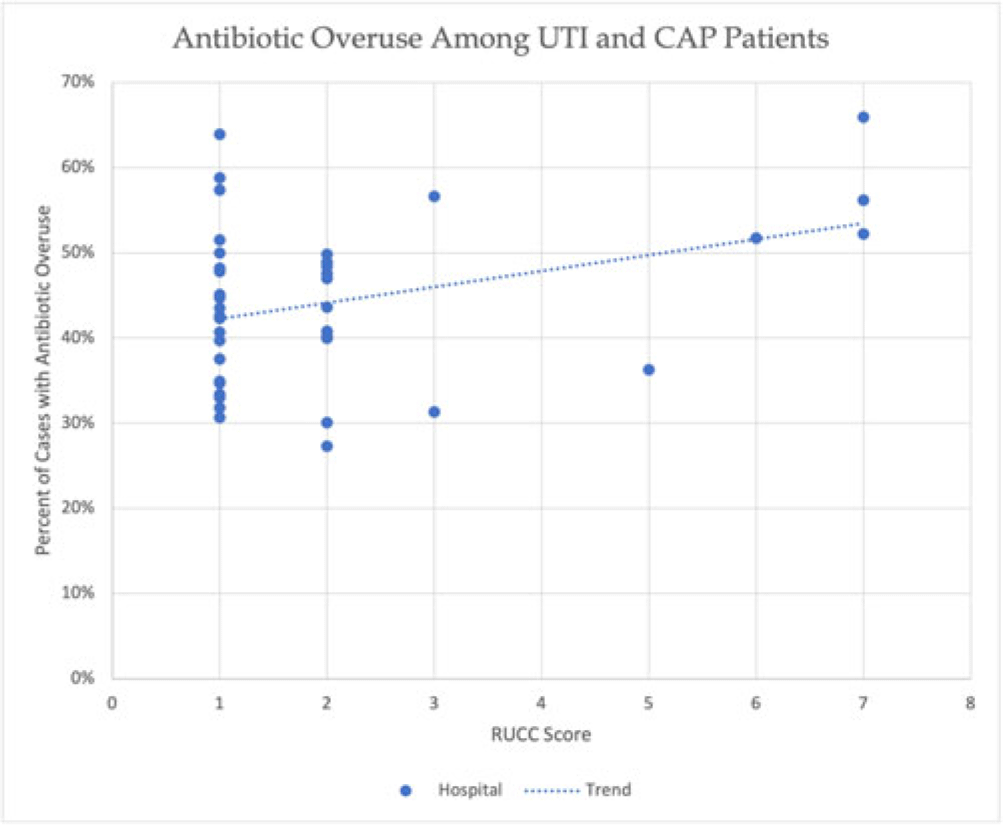
Background: Antibiotic overuse and the resulting patient outcomes span all hospitals. However, although antibiotic stewardship can improve antibiotic use, effective stewardship programs require expertise and an infrastructure that are not present in all hospitals. Rural hospitals have less access to resources, infectious disease expertise, and participation in academic research. Thus, we compared antibiotic overuse at discharge between rural and nonrural hospitals for patients diagnosed with community-associated pneumonia (CAP) or urinary tract infection (UTI)—the 2 most common hospital infections. Methods: To determine whether antibiotic overuse at discharge was higher among rural versus nonrural hospitals, we analyzed data from a 41-hospital prospective cohort of patients treated for CAP or UTI between July 1, 2017, and July 30, 2019, in Michigan. Antibiotic overuse was defined as treatment that was unnecessary (ie, patient did not have an infection), excessive (ie, duration >4 days for CAP), or included suboptimal fluoroquinolone use (ie, safer alternative available). Overuse was determined based on patient risk factors, symptoms, allergies, diagnostic results, and time to stability. Hospital rurality was defined using the Rural–Urban Continuum Codes (RUCC) score. We defined rural as a score ≥4 and very rural as a score of 7–9. We used t tests to compare the mean percentage of patients with antibiotic overuse at discharge between nonrural and rural (and very rural) hospitals. Results: Across 41 hospitals, we included 23,449 patients with CAP or UTI. There were 5 rural (and 3 very rural) hospitals with 2,039 (and 1,082) patients. Antibiotic overuse at discharge was present in 43.1% of patient cases in nonrural hospitals, 52.5% in rural hospitals (P = .04 vs nonrural) and 58.1% in very rural hospitals (P = .007 vs nonrural). Compared to nonrural hospitals, the mean percentage of cases with antibiotic overuse at discharge in rural hospitals was 9.4% higher (15.1% higher in very rural hospitals). Results were similar in a subgroup analysis of only patients with UTI (47.0% in rural vs 37.5% in nonrural, mean difference, 9.5%; P = .03) but were not statistically significant in patients with CAP (53.8% vs 48.0%, respectively; mean difference, 5.8%; P = 0.23). Conclusions: In this retrospective study, rural hospitals—especially very rural hospitals, had higher rates of antibiotic overuse at discharge than nonrural hospitals. Our findings suggest that antibiotic stewardship interventions tailored toward the unique differences in infrastructure, resources, and needs of rural hospitals are essential to community health.
Disclosures: None
Three-day antibiotic duration in patients with pneumonia: A sixty-eight–hospital cohort
- Valerie Vaughn, Lindsay Petty, David Ratz, Elizabeth McLaughlin, Tawny Czilok, Jennifer Horowitz, Anurag Malani, Danielle Osterholzer, Scott Flanders, Tejal Gandhi
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s22
-
- Article
-
- You have access Access
- Open access
- Export citation
-
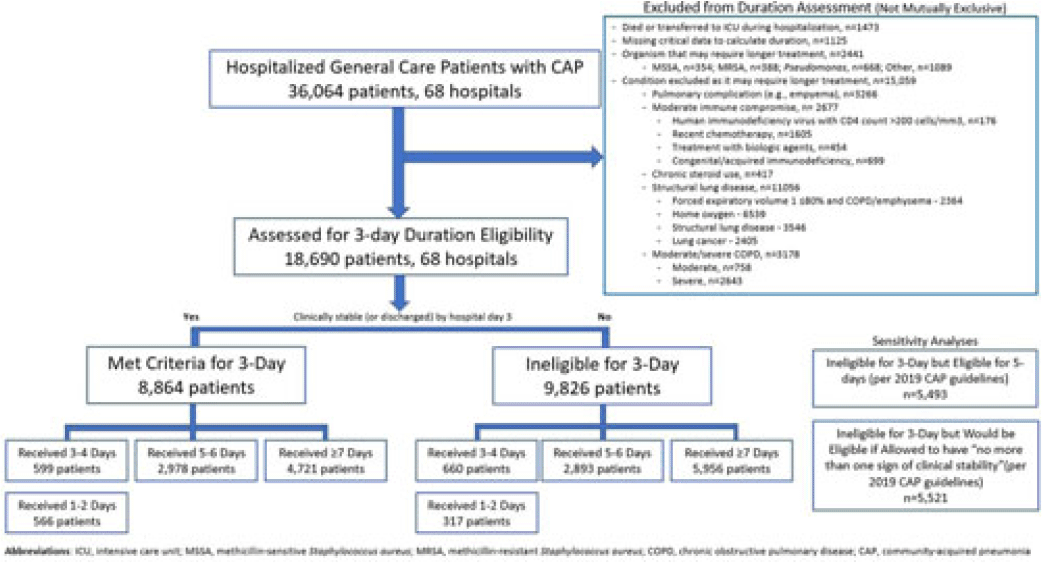
Background: Since 2019, community-acquired pneumonia (CAP) guidelines have recommended hospitalized patients be treated until clinical “stability and for no less than 5 days.” However, randomized trials have reported that, in patients who stabilize by hospital day 3, very short antibiotic durations (eg, 3 days) are noninferior to longer durations. How these trial results relate to real-world practice is unknown. Methods: Using a 68-hospital cohort study of hospitalized, general-care adults with CAP, we aimed to (1) quantify the percentage of patients who—according to trial criteria—qualify for a 3-day antibiotic duration, (2) quantify the percentage who actually received a 3-day duration, and (3) assess 30-day outcomes. Patients were considered to have CAP if they had a pneumonia discharge diagnosis and met clinical criteria for CAP. Patients with concomitant infections (including COVID-19), admission to intensive care, or severe immunocompromise were not included. Results: Between February 23, 2017, and August 3, 2022, 36,064 patients with CAP were included. Of those, 48.2% (9,826 of 36,064) were excluded due to a condition or organism ineligible for the 3-day treatment (Fig. 1). Of the 18,690 patients remaining, 52.6% (9,826) were unstable on day 3 and thus were ineligible for the 3-day treatment. Therefore, of all 36,064 patients, only 8,864 (24.6%) would be eligible under trial criteria for a 3-day treatment. Notably, 5,493 (55.9%) of 9,826 patients unstable on day 3 would be eligible for 5 days of treatment under national guidelines. In practice, use of 3–4-day treatment was rare, occurring in 599 (6.8%) of 8,864 patients eligible for a 3-day treatment versus 660 (6.7%) of 9,826 patients unstable on day 3 (P = .945). Use of 3–4-day treatment increased over time and comorbidities that could mimic CAP or a negative procalcitonin were more common in patients who received a 3–4-day treatment whereas specific symptoms of CAP were less common (Fig. 2). After adjustments, patients eligible for a 3-day duration who received a 3–4 day treatment versus a ≥5-day treatment had higher 30-day mortality (aOR, 1.87; 95% CI, 1.32–2.64) and readmission (aOR, 1.35; 95% CI, 1.17–1.56). Conclusions: Across 68 hospitals, <25% of patients hospitalized with CAP would be eligible for a 3-day antibiotic treatment. Though increasing over time, there was little use of 3–4-day treatments and, when prescribed, outcomes were worse, potentially due to CAP misdiagnosis. Given the small number of patients eligible for 3-day treatment, and the potential harm with too-short durations, it may be prudent to focus on increasing the use of 5-day treatments.
Disclosures: None
Risk Factors and outcomes associated with inappropriate empiric broad-spectrum antibiotic use in hospitalized patients with community-acquired pneumonia
- Tejal Gandhi, Lindsay Petty, Valerie Vaughn, Anurag Malani, David Ratz, Tawny Czilok, Jennifer Horowitz, Elizabeth McLaughlin, Lisa Dumkow, Stephanie Burdick, Danielle Osterholzer, Mariam Younas, Steven Bernstein, Scott Flanders
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s31-s32
-
- Article
-
- You have access Access
- Open access
- Export citation
-
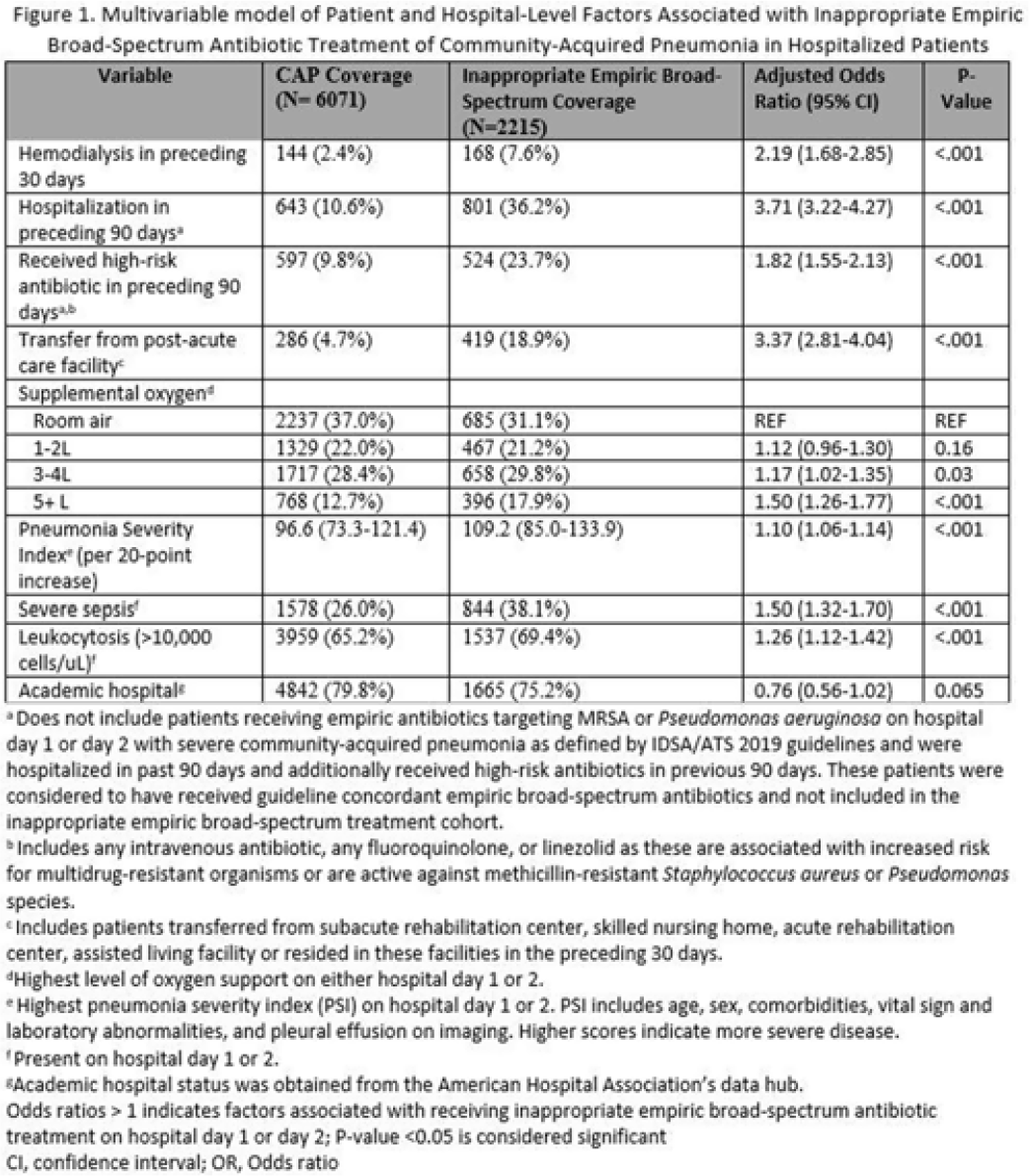
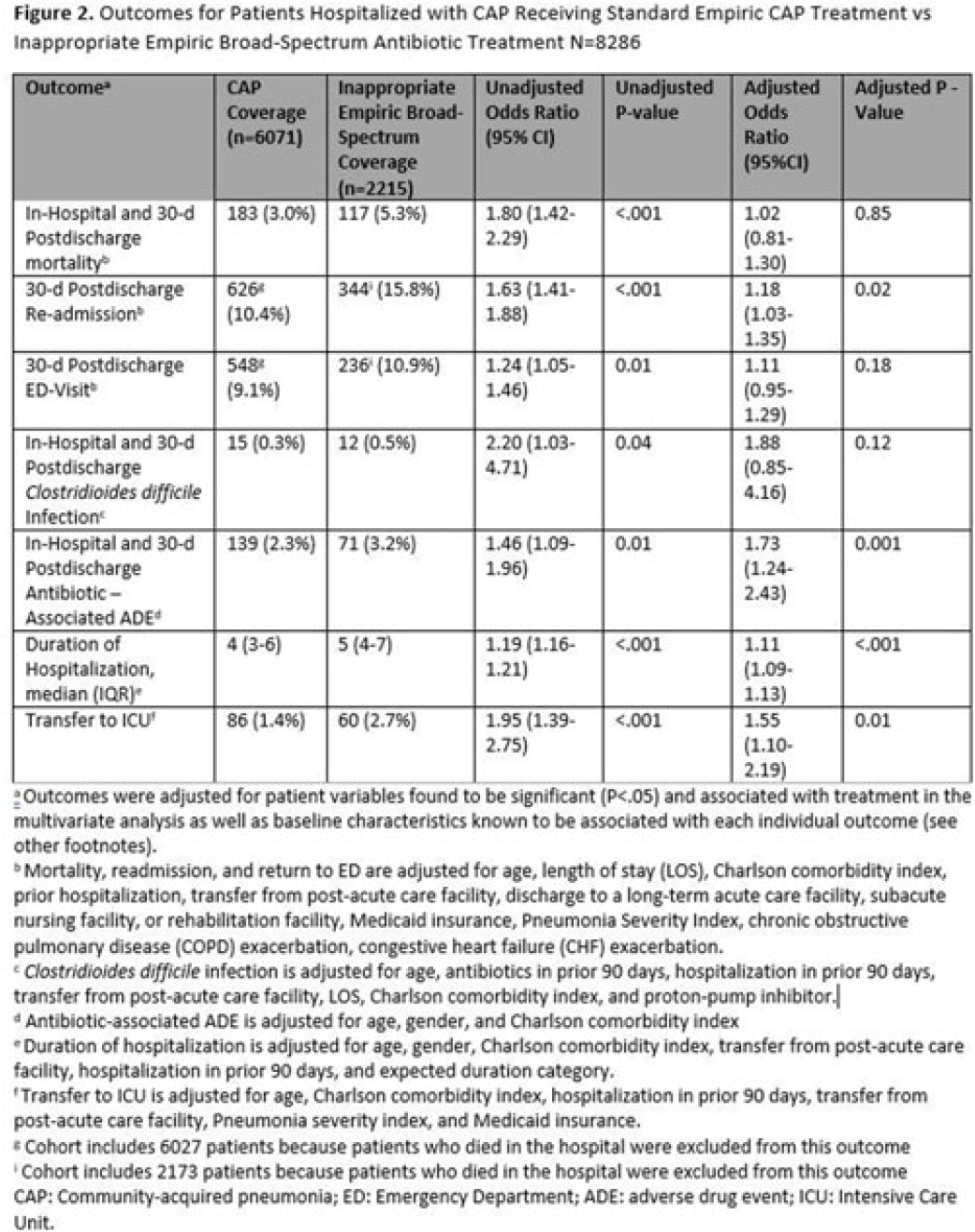
Background: Inappropriate broad-spectrum antibiotic use targeting methicillin-resistant Staphylococcus aureus (MRSA) and Pseudomonas aeruginosa can result in increased adverse events, antibiotic resistance, and Clostridioides difficile infection. In 2019, revised ATS/IDSA community-acquired pneumonia (CAP) guidelines removed healthcare-associated pneumonia (HCAP) as a clinical entity and modified patient factors warranting empiric broad-spectrum antibiotic (BSA) use. As a result, most patients hospitalized with CAP should receive empiric antibiotics targeting standard CAP pathogens. Based on revised guidelines, we evaluated predictors and outcomes associated with inappropriate BSA use among hospitalized patients with CAP. Methods: Between November 2019 and July 2022, trained abstractors collected data on non-ICU adult medical patients admitted with CAP at 67 Michigan hospitals who received either an inappropriate empiric BSA on hospital day 1 or 2 or a standard CAP regimen. Inappropriate empiric BSA use was defined as use of an anti-MRSA or anti-pseudomonal antibiotic in a patient eligible for standard CAP coverage per IDSA guidelines. Patients with immune compromise, moderate or severe chronic obstructive pulmonary disease (COPD), pulmonary complication, or guideline-concordant treatment with BSA were excluded. Data collected included comorbidities, antibiotic use and hospitalizations in the preceding 90 days, cultures in the preceding year, signs or symptoms of pneumonia, hospital characteristics, and 30-day postdischarge patient outcomes. Data were collected through chart review and patient phone calls. Predictors of inappropriate empiric BSA were evaluated using logistic general estimating equation (GEE) models, accounting for hospital-level clustering. We assessed the effect of inappropriate empiric BSA (vs standard CAP therapy) on 30-day patient outcomes using logistic GEE models controlling for predictors associated with the outcome and probability of treatment. Results: Of 8,286 included patients with CAP, 2,215 (26.7%) were empirically treated with inappropriate BSA. The median BSA treatment was 3 days (IQR, 2.5). After adjustments, factors associated with inappropriate empiric BSA treatment included hospitalization or treatment with high-risk antibiotics in preceding 90 days, transfer from a postacute care facility, hemodialysis, support with ≥3 L supplemental oxygen, severe sepsis, leukocytosis, and higher pneumonia severity index (Fig. 1). After adjustments, patients with inappropriate empiric BSA treatment had higher readmissions 30 days after discharge, more transfers to the intensive care unit, more antibiotic-associated adverse events, and longer hospitalizations (Fig. 2). Conclusions: Patients hospitalized with CAP often received inappropriate BSA as empiric coverage, and this inappropriate antibiotic selection was associated with worse patient outcomes. To improve patient outcomes, stewardship efforts should focus on reducing inappropriate BSA use in patients hospitalized for CAP with historic HCAP risk factors or severe CAP without other guideline-directed indications for BSA.
Financial support. H.M.S. initiative is underwritten by Blue Cross and Blue Shield of Michigan.
Disclosures: None
Duties, resources, and burnout of antibiotic stewards during the coronavirus disease 2019 (COVID-19) pandemic
- Valerie M. Vaughn, Guinn E. Dunn, Jennifer K. Horowitz, Elizabeth S. McLaughlin, Tejal N. Gandhi
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 05 November 2021, e39
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
Risk factors and outcomes associated with community-onset and hospital-acquired coinfection in patients hospitalized for coronavirus disease 2019 (COVID-19): A multihospital cohort study
- Part of
- Lindsay A. Petty, Scott A. Flanders, Valerie M. Vaughn, David Ratz, Megan O’Malley, Anurag N. Malani, Laraine Washer, Tae Kim, Keith E. Kocher, Scott Kaatz, Tawny Czilok, Elizabeth McLaughlin, Hallie C. Prescott, Vineet Chopra, Tejal Gandhi
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 9 / September 2022
- Published online by Cambridge University Press:
- 26 July 2021, pp. 1184-1193
- Print publication:
- September 2022
-
- Article
- Export citation
-
Background:
We sought to determine the incidence of community-onset and hospital-acquired coinfection in patients hospitalized with coronavirus disease 2019 (COVID-19) and to evaluate associated predictors and outcomes.
Methods:In this multicenter retrospective cohort study of patients hospitalized for COVID-19 from March 2020 to August 2020 across 38 Michigan hospitals, we assessed prevalence, predictors, and outcomes of community-onset and hospital-acquired coinfections. In-hospital and 60-day mortality, readmission, discharge to long-term care facility (LTCF), and mechanical ventilation duration were assessed for patients with versus without coinfection.
Results:Of 2,205 patients with COVID-19, 141 (6.4%) had a coinfection: 3.0% community onset and 3.4% hospital acquired. Of patients without coinfection, 64.9% received antibiotics. Community-onset coinfection predictors included admission from an LTCF (OR, 3.98; 95% CI, 2.34–6.76; P < .001) and admission to intensive care (OR, 4.34; 95% CI, 2.87–6.55; P < .001). Hospital-acquired coinfection predictors included fever (OR, 2.46; 95% CI, 1.15–5.27; P = .02) and advanced respiratory support (OR, 40.72; 95% CI, 13.49–122.93; P < .001). Patients with (vs without) community-onset coinfection had longer mechanical ventilation (OR, 3.31; 95% CI, 1.67–6.56; P = .001) and higher in-hospital mortality (OR, 1.90; 95% CI, 1.06–3.40; P = .03) and 60-day mortality (OR, 1.86; 95% CI, 1.05–3.29; P = .03). Patients with (vs without) hospital-acquired coinfection had higher discharge to LTCF (OR, 8.48; 95% CI, 3.30–21.76; P < .001), in-hospital mortality (OR, 4.17; 95% CI, 2.37–7.33; P ≤ .001), and 60-day mortality (OR, 3.66; 95% CI, 2.11–6.33; P ≤ .001).
Conclusion:Despite community-onset and hospital-acquired coinfection being uncommon, most patients hospitalized with COVID-19 received antibiotics. Admission from LTCF and to ICU were associated with increased risk of community-onset coinfection. Future studies should prospectively validate predictors of COVID-19 coinfection to facilitate the reduction of antibiotic use.
Antibiotic Overuse at Discharge in Hospitalized Patients with Bacteriuria or Treated for Pneumonia: A Multihospital Study
- Valerie M Vaughn, Lindsay A. Petty, Tejal N. Gandhi, Keith S. Kaye, Anurag Malani, Steven J. Bernstein, David Ratz, Elizabeth McLaughlin, Scott A. Flanders
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s459-s461
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Nearly half of hospitalized patients with bacteriuria or treated for pneumonia receive unnecessary antibiotics (noninfectious or nonbacterial syndrome such as asymptomatic bacteriuria), excess duration (antibiotics prescribed for longer than necessary), or avoidable fluoroquinolones (safer alternative available) at hospital discharge.1–3 However, whether antibiotic overuse at discharge varies between hospitals or is associated with patient outcomes remains unknown. Methods: From July 2017 to December 2018, trained abstractors at 46 Michigan hospitals collected detailed data on a sample of adult, non–intensive care, hospitalized patients with bacteriuria (positive urine culture with or without symptoms) or treated for community-acquired pneumonia (CAP; includes those with the disease formerly known as healthcare-associated pneumonia [HCAP]). Antibiotic prescriptions at discharge were assessed for antibiotic overuse using a previously described, guideline-based hierarchical algorithm.3 Here, we report the proportion of patients discharged with antibiotic overuse by the hospital. We also assessed hospital-level correlation (using Pearson’s correlation coefficient) between antibiotic overuse at discharge for patients with bacteriuria and patients treated for CAP. Finally, we assessed the association of antibiotic overuse at discharge with patient outcomes (mortality, readmission, emergency department visit, and antibiotic-associated adverse events) at 30 days using logit generalized estimating equations adjusted for patient characteristics and probability of treatment. Results: Of 17,081 patients (7,207 with bacteriuria; 9,874 treated for pneumonia), nearly half (42.2%) had antibiotic overuse at discharge (36.3% bacteriuria and 51.1% pneumonia). The percentage of patients discharged with antibiotic overuse varied 5-fold among hospitals from 14.7% (95% CI, 8.0%–25.3%) to 74.3% (95% CI, 64.2%–83.8%). Hospital rates of antibiotic overuse at discharge were strongly correlated between bacteriuria and CAP (Pearson’s correlation coefficient, 0.76; P ≤ .001) (Fig. 1). In adjusted analyses, antibiotic overuse at discharge was not associated with death, readmission, emergency department visit, or Clostridioides difficile infection. However, each day of overuse was associated with a 5% increase in the odds of patient-reported antibiotic-associated adverse events after discharge (Fig. 2). Conclusions: Antibiotic overuse at discharge was common, varied widely between hospitals, and was associated with patient harm. Furthermore, antibiotic overuse at discharge was strongly correlated between 2 disparate diseases, suggesting that prescribing culture or discharge processes—rather than disease-specific factors—contribute to overprescribing at discharge. Thus, discharge stewardship may be needed to target multiple diseases.
Funding: This study was supported by the Society for Healthcare Epidemiology of America and by Blue Cross Blue Shield of Michigan and Blue Care Network.
Disclosures: Valerie M. Vaughn reports contracted research for Blue Cross and Blue Shield of Michigan, the Department of VA, the NIH, the SHEA, and the APIC. She also reports receipt of funds from the Gordon and Betty Moore Foundation Speaker’s Bureau, the CDC, the Pew Research Trust, Sepsis Alliance, and the Hospital and Health System Association of Pennsylvania.
Misdiagnosis of Urinary Tract Infection Linked to Misdiagnosis of Pneumonia: A Multihospital Cohort Study
- Valerie M. Vaughn, Ashwin Gupta, Lindsay A. Petty, Tejal N. Gandhi, Scott A. Flanders, Lakshmi Swaminathan, Lama Hsaiky, Lama Hsaiky, David Ratz, Jennifer Horowitz, Elizabeth McLaughlin, Vineet Chopra
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s488-s489
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Clinicians often diagnose bacterial infections such as urinary tract infection (UTI) and pneumonia in patients who are asymptomatic or have nonbacterial causes of their symptoms. Misdiagnosis of infection leads to unnecessary antibiotic use and potentially delays correct diagnoses. Interventions to improve diagnosis often focus on infections separately. However, if misdiagnosis is linked, broader interventions to improve diagnosis may be more effective. Thus, we assessed whether misdiagnosis of UTI and community-acquired pneumonia (CAP) was correlated. Methods: From July 2017 to July 2019, abstractors at 46 Michigan hospitals collected data on a sample of adult, non–intensive care, hospitalized patients with bacteriuria (positive urine culture) or who were treated for presumed CAP (discharge diagnosis plus antibiotics). Patients with concomitant bacterial infections were excluded. Using a previously described method,1,2 patients were assessed for UTI or CAP based on symptoms, signs, and laboratory or radiology findings. Misdiagnosis of UTI was defined as patients with asymptomatic bacteriuria (ASB) treated with antibiotics number of patients with bacteriuria Misdiagnosis of CAP was defined as patients treated for presumed CAP who did not have CAP number of patients treated for presumed CAP. Hospital-level correlation was assessed using Pearson’s correlation coefficient between misdiagnosis of UTI and CAP. For patients with prescriber data (N = 3,293), we also assessed emergency department (ED)-level correlation. Results: Of 11,914 patients with bacteriuria, 31.9% (N = 3,796) had ASB. Of those, 2,973 of 3,796 (78.3%) received antibiotics. Of 14,085 patients treated for CAP, 1,602 (11.4%) did not have CAP. Incidence of misdiagnosis varied by hospital: those with high rates of misdiagnosis of UTI were more likely to have high rates of misdiagnosis of CAP (Pearson’s correlation coefficient, 0.58; P ≤ .001) (Fig. 1). Of 2,137 patients misdiagnosed with UTI, 1,159 (54.2%) had antibiotic treatment started in the ED; of those, 942 (81.3%) remained on antibiotics on day 3 of hospitalization. Of 1,156 patients misdiagnosed with CAP, 871 (75.3%) had antibiotic therapy started in the ED, and 789 of these 871 patients (90.6%) were still on antibiotics on day 3 of hospitalization. Hospitals with high rates of UTI misdiagnosis in the ED were more likely to have high rates of CAP misdiagnosis in the ED (Pearson’s correlation coefficient, 0.33; P ≤ .001). Conclusions: Misdiagnosis of 2 unrelated infections was moderately correlated by hospital and weakly correlated by hospital ED. Potential causes include differences in organizational culture (eg, low tolerance for diagnostic uncertainty, emergency department culture), organizational initiatives (eg, sepsis, stewardship), or coordination between emergency and hospital medicine. Additionally, antibiotics initiated in the ED were typically continued following admission, potentially reflecting diagnosis momentum.
Funding: This work was supported by Blue Cross Blue Shield of Michigan and Blue Care Network.
Disclosures: Valerie M. Vaughn reports contract research for Blue Cross and Blue Shield of Michigan, the Department of Veterans’ Affairs, the NIH, the SHEA, and the APIC. She also reports fees from the Gordon and Betty Moore Foundation Speaker’s Bureau, the CDC, the Pew Research Trust, Sepsis Alliance, and The Hospital and Health System Association of Pennsylvania.
The Ontario Neurodegenerative Disease Research Initiative (ONDRI)
- Sali M. K. Farhan, Robert Bartha, Sandra E. Black, Dale Corbett, Elizabeth Finger, Morris Freedman, Barry Greenberg, David A. Grimes, Robert A. Hegele, Chris Hudson, Peter W. Kleinstiver, Anthony E. Lang, Mario Masellis, William E. McIlroy, Paula M. McLaughlin, Manuel Montero-Odasso, David G. Munoz, Douglas P. Munoz, Stephen Strother, Richard H. Swartz, Sean Symons, Maria Carmela Tartaglia, Lorne Zinman, ONDRI Investigators, Michael J. Strong
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 44 / Issue 2 / March 2017
- Published online by Cambridge University Press:
- 22 December 2016, pp. 196-202
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Because individuals develop dementia as a manifestation of neurodegenerative or neurovascular disorder, there is a need to develop reliable approaches to their identification. We are undertaking an observational study (Ontario Neurodegenerative Disease Research Initiative [ONDRI]) that includes genomics, neuroimaging, and assessments of cognition as well as language, speech, gait, retinal imaging, and eye tracking. Disorders studied include Alzheimer’s disease, amyotrophic lateral sclerosis, frontotemporal dementia, Parkinson’s disease, and vascular cognitive impairment. Data from ONDRI will be collected into the Brain-CODE database to facilitate correlative analysis. ONDRI will provide a repertoire of endophenotyped individuals that will be a unique, publicly available resource.
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
Dietary N-nitroso compounds and risk of colorectal cancer: a case–control study in Newfoundland and Labrador and Ontario, Canada
- Yun Zhu, Peizhon Peter Wang, Jing Zhao, Roger Green, Zhuoyu Sun, Barbara Roebothan, Josh Squires, Sharon Buehler, Elizabeth Dicks, Jinhui Zhao, Michelle Cotterchio, Peter T. Campbell, Meera Jain, Patrick S. Parfrey, John R. Mclaughlin
-
- Journal:
- British Journal of Nutrition / Volume 111 / Issue 6 / 28 March 2014
- Published online by Cambridge University Press:
- 25 October 2013, pp. 1109-1117
- Print publication:
- 28 March 2014
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Several N-nitroso compounds (NOC) have been shown to be carcinogenic in a variety of laboratory animals, but evidence of their carcinogenicity in humans is lacking. We aimed to examine the association between NOC intake and colorectal cancer (CRC) risk and possible effect modification by vitamins C and E and protein in a large case–control study carried out in Newfoundland and Labrador and Ontario, Canada. A total of 1760 case patients with pathologically confirmed adenocarcinoma and 2481 population controls were asked to complete a self-administered FFQ to evaluate their dietary intakes 1 year before diagnosis (for cases) or interview (for controls). Adjusted OR and 95 % CI were calculated across the quintiles of NOC (measured by N-nitrosodimethylamine (NDMA)) intake and relevant food items using unconditional logistic regression. NDMA intake was found to be associated with a higher risk of CRC (highest v. lowest quintiles: OR 1·42, 95 % CI 1·03, 1·96; P for trend = 0·005), specifically for rectal carcinoma (OR 1·61, 95 % CI 1·11, 2·35; P for trend = 0·01). CRC risk also increased with the consumption of NDMA-containing meats when the highest tertile was compared with the lowest tertile (OR 1·47, 95 % CI 1·03, 2·10; P for trend = 0·20). There was evidence of effect modification between dietary vitamin E and NDMA. Individuals with high NDMA and low vitamin E intakes had a significantly increased risk than those with both low NDMA and low vitamin E intakes (OR 3·01, 95 % CI 1·43, 6·51; P for interaction = 0·017). The present results support the hypothesis that NOC intake may be positively associated with CRC risk in humans. Vitamin E, which inhibits nitrosation, could modify the effect of NDMA on CRC risk.
Mesolithic and Neolithic Human Remains from Foxhole Cave, Gower, South Wales
- Rick Schulting, Linda Fibiger, Richard Macphail, Rowan McLaughlin, Emily Murray, Catherine Price, Elizabeth A Walker
-
- Journal:
- The Antiquaries Journal / Volume 93 / September 2013
- Published online by Cambridge University Press:
- 20 September 2013, pp. 1-23
- Print publication:
- September 2013
-
- Article
- Export citation
-
This paper presents an overview of the results of two brief excavation seasons (2008 and 2010) at Foxhole Cave, Gower, south Wales, placing them into the wider context of mid-Holocene Britain. No prehistoric pottery was found and the few pieces of worked flint recovered are diagnostic of the Mesolithic period. Typically for the Carboniferous limestone caves of Gower, bone was well preserved, however, and though much of the material in the heavily disturbed upper metre or so of the deposits was modern sheep and rabbit, scattered fragments representing the remains of at least six humans were also recovered, of which two have been directly radiocarbon-dated using accelerator mass spectrometry (AMS 14C) to the Late Mesolithic and two to the earlier Neolithic (the remaining two providing Romano-British and medieval dates). Their associated stable carbon and nitrogen isotope values indicate a significant difference in diet between the two periods (contrary to the results from an earlier excavation in 1997), with marine foods contributing around half of the protein for the Mesolithic individuals and little or none for the Neolithic individuals. The new results are consistent with those from Caldey Island, Pembrokeshire, some 30km to the west. The floor of the cave has still not been reached at around 2m depth; limited investigation of the lowermost levels has yielded a Pleistocene fauna (including reindeer, aurochs or bison and collared lemming) with dates back to approx 33,500 cal bc, though with no definite evidence for human activity so far. A small, dark-stained fragment of human cranium was recovered from what may be pre-Holocene levels, but this failed to produce sufficient collagen for dating. In addition to a marked dietary shift, the combined stable isotope and dating programme provides further support for an equally striking temporal gap of some two millennia between the Mesolithic and Neolithic use of caves for burial.
Contributors
-
- By Núria Duran Adroher, Sergio Aguilar-Gaxiola, Jordi Alonso, Ali Obaid Al-Hamzawi, Laura Helena Andrade, Matthias C. Angermeyer, James Anthony, Corina Benjet, Guilherme Borges, Joshua Breslau, Evelyn J. Bromet, Ronny Bruffaerts, Brendan Bunting, Huibert Burger, José Miguel Caldas de Almeida, Graça Cardoso, Somnath Chatterji, Wai Tat Chiu, Giovanni de Girolamo, Ron de Graaf, Peter de Jonge, Koen Demyttenaere, John Fayyad, Alize J. Ferrari, Silvia Florescu, Anne M. Gadermann, Meyer Glantz, Jen Green, Michael J. Gruber, Oye Gureje, Josep Maria Haro, Yanling He, Steven G. Heeringa, Hristo Hinkov, Chiyi Hu, Yueqin Huang, Irving Hwang, Robert Jin, Elie G. Karam, Norito Kawakami, Ronald C. Kessler, Lola Kola, Viviane Kovess-Masféty, Michael C. Lane, Carmen Lara, William LeBlanc, Sing Lee, Jean-Pierre Lépine, Daphna Levinson, Zhaorui Liu, Gustavo Loera, Herbert Marschinger, Katie A. McLaughlin, Maria Elena Medina-Mora, Elizabeth Miller, Samuel D. Murphy, Aimee Nasser Karam, Matthew K. Nock, Mark A. Oakley Browne, Siobhan O’Neill, Johan Ormel, Beth-Ellen Pennell, Maria V. Petukhova, José Posada-Villa, Rajesh Sagar, Mohammad Salih Khalaf, Nancy A. Sampson, Kathleen Saunders, Michael Schoenbaum, Kate M. Scott, Soraya Seedat, Victoria Shahly, Dan J. Stein, Hisateru Tachimori, Nezar Ismet Taib, Adley Tsang, T. Bedirhan Üstün, Maria Carmen Viana, Gemma Vilagut, Michael R. Von Korff, J. Elisabeth Wells, Harvey A. Whiteford, David R. Williams, Ben Wu, Miguel Xavier, Alan M. Zaslavsky
- Edited by Jordi Alonso, Universitat Pompeu Fabra, Barcelona, Somnath Chatterji, World Health Organization, Geneva, Yanling He
-
- Book:
- The Burdens of Mental Disorders
- Print publication:
- 09 May 2013, pp ix-xii
-
- Chapter
- Export citation
Contributors
-
- By R. J. Aitken, Gokhan Akkoyunlu, David F. Albertini, Christiani A. Amorim, R. A. Anderson, Baris Ata, Pedro N. Barri, Mohamed A. Bedaiwy, Rosita Bergström, Veronica Bianchi, Montserrat Boada, Paolo Boffetta, Andrea Borini, Karina Braga Ribeiro, Peter R. Brinsden, Ralph L. Brinster, Jason G. Bromer, A. L. Caplan, Chian Ri-Cheng, Ina N. Cholst, A. Ciobanu, Megan Clowse, Ana Cobo, Susannah C. Copland, John K. Critser, B. J. Curry, Giuseppe Del Priore, M. De Vos, Marie-Madeleine Dolmans, Javier Domingo, Jacques Donnez, David H. Edgar, Nanette R. Elster, Carol Fabian, Gregory M. Fahy, Tommaso Falcone, Debra Friedman, Jill P. Ginsberg, Debra A. Gook, Julie R. Gralow, Elizabeth Grill, Sebastien Gouy, Xu Han, Lisa M. Harlan-Williams, Outi Hovatta MD, Wayland Hsiao, Zhongwei Huang, E. Isachenko, V. Isachenko, Roy A. Jensen, I. I. Katkov, S. Samuel Kim, Jennifer Klemp, Larissa A. Korde, R. Kreienberg, Srinivasan Krishnamurthy, Juergen Liebermann, J. Ryan Martin, Elizabeth A. McGee, Marie McLaughlin, P. Mathevet, D. Meirow, Philippe Morice, Steven F. Mullen, Kutluk Oktay, Pasquale Patrizio, Antonio Pellicer, Pinki K. Prasad, Kenny A. Rodriguez-Wallberg, Erin Rohde, Allison B. Rosen, Zev Rosenwaks, María Sánchez, R. Sanchez, Glenn L. Schattman, Peter N. Schlegel, Einat Shalom-Paz, Lonnie D. Shea, Gunapala Shetty, Jill Simmons, Carrie A. Smith, J. Smitz, Miquel Solé, Jean Squifflet, Shane R. Stecklein, Jerome F. Strauss, David J. Tagler, Seang Lin Tan, Evelyn E. Telfer, Sreedhar Thirumala, Michael J. Tucker, Catherine Uzan, Anne Van Langendonckt, Anna Veiga, W. H. B. Wallace, Wenjia Wang, Brent Waters, Dagan Wells, Teresa K. Woodruff, Erik Woods, Christine Wyns
- Edited by Jacques Donnez, Université Catholique de Louvain, Belgium, S. Samuel Kim, University of Kansas
-
- Book:
- Principles and Practice of Fertility Preservation
- Published online:
- 04 February 2011
- Print publication:
- 03 February 2011, pp x-xiv
-
- Chapter
- Export citation
Point prevalence of diabetes, obesity, hyperlipidaemia, hypertension and smoking in outpatients on clozapine
- Larkin Feeney, Fiona Kelly, Judy Lee, Elizabeth Kelly, Sheila McLaughlin, James H O'Boyle
-
- Journal:
- Irish Journal of Psychological Medicine / Volume 24 / Issue 2 / June 2007
- Published online by Cambridge University Press:
- 13 June 2014, pp. 59-61
- Print publication:
- June 2007
-
- Article
- Export citation
-
Objectives: Patients with schizophrenia are known to be at higher risk than the general population of cardiovascular disease. Clozapine has been associated in the literature with high levels of cardiovascular risk factors such as weight gain, diabetes, hyperlipidaemia and hypertension. We set out to determine the prevalence of these risk factors in a population of Irish psychiatric patients.
Method: In February 2006 we measured body mass index, fasting blood glucose, haemoglobin A1c (HbA1c), lipid levels, mean blood pressure and smoking rates among all outpatients prescribed clozapine attending an urban, community based mental health service.
Results: There were 50 outpatients (33 male; 17 female) on clozapine and they had been taking it for a mean of 5.4 years (mean daily dose 428.8mg). The mean body mass index was 28.3. Patients had gained a mean of 8kg since commencing clozapine. One patient had been diagnosed with diabetes. Of the other 49 none met diagnostic criteria for diabetes. The mean fasting blood glucose was 5.5mmol/l and the mean HbA1c was 5.7%. One patient was on treatment for hyperlipidaemia. The mean fasting cholesterol among the other 49 patients was 5.4mmol/l, while the mean fasting triglycerides was 2.1 mmol/l. Thirty (61.2%) had a fasting cholesterol greater than 5.0mmol/l, while 18 (36.7%) had triglycerides of greater than 2.0mmol/l. Three patients were on treatment for hypertension. Thirty-six of the 50 (72%) smoked (mean 13 cigarettes per day).
Conclusions: The prevalence of obesity, diabetes, hyperlipidaemia and hypertension in this population was high but lower than might have been expected from US studies. It is important that cardiovascular risk factors are closely monitored and actively addressed in this at risk population.
Contributions of parental alcoholism, prenatal substance exposure, and genetic transmission to child ADHD risk: a female twin study
- VALERIE S. KNOPIK, ELIZABETH P. SPARROW, PAMELA A. F. MADDEN, KATHLEEN K. BUCHOLZ, JAMES J. HUDZIAK, WENDY REICH, WENDY S. SLUTSKE, JULIA D. GRANT, TARA L. McLAUGHLIN, ALEXANDRE TODOROV, RICHARD D. TODD, ANDREW C. HEATH
-
- Journal:
- Psychological Medicine / Volume 35 / Issue 5 / May 2005
- Published online by Cambridge University Press:
- 06 January 2005, pp. 625-635
-
- Article
- Export citation
-
Background. Genetic influences have been shown to play a major role in determining the risk of attention-deficit hyperactivity disorder (ADHD). In addition, prenatal exposure to nicotine and/or alcohol has also been suggested to increase risk of the disorder. Little attention, however, has been directed to investigating the roles of genetic transmission and prenatal exposure simultaneously.
Method. Diagnostic telephone interview data from parents of Missouri adolescent female twin pairs born during 1975–1985 were analyzed. Logistic regression models were fitted to interview data from a total of 1936 twin pairs (1091 MZ and 845 DZ pairs) to determine the relative contributions of parental smoking and drinking behavior (both during and outside of pregnancy) as risk factors for DSM-IV ADHD. Structural equation models were fitted to determine the extent of residual genetic and environmental influences on ADHD risk while controlling for effects of prenatal and parental predictors on risk.
Results. ADHD was more likely to be diagnosed in girls whose mothers or fathers were alcohol dependent, whose mothers reported heavy alcohol use during pregnancy, and in those with low birth weight. Controlling for other risk factors, risk was not significantly increased in those whose mothers smoked during pregnancy. After allowing for effects of prenatal and childhood predictors, 86% of the residual variance in ADHD risk was attributable to genetic effects and 14% to non-shared environmental influences.
Conclusions. Prenatal and parental risk factors may not be important mediators of influences on risk with much of the association between these variables and ADHD appearing to be indirect.
The heterobasidiomycete moss parasites Jola and Eocronartium in culture: cytology, ultrastructure, and anamorph
- Elizabeth M. FRIEDERS, David J. MCLAUGHLIN
-
- Journal:
- Mycological Research / Volume 105 / Issue 6 / June 2001
- Published online by Cambridge University Press:
- 12 July 2001, pp. 734-744
- Print publication:
- June 2001
-
- Article
- Export citation
-
The heterobasidiomycete moss parasites Eocronartium and Jola have figured prominently in theories of the evolution of the rust fungi and of the basidiomycetes. Such theories made implicit assumptions about the moss parasites, although very little of their life history was known. This is the first in a series of studies to elucidate the life history of the moss parasites. Polyspore monokaryotic cultures were obtained from basidiospores, and dikaryotic cultures were obtained from hyphae inside the moss host plant. In culture, the moss parasites produced Sporothrix-like anamorphs. The uninucleate conidia germinated by a germ tube, by production of single secondary conidia, or by iterative germination. Conidial-hyphal fusion was observed. A dikaryon was produced by mating single conidial isolates of Eocronartium muscicola, completing a part of its life history. Ultrastructural characteristics of wall break at branching, condensed chromatin during interphase, and simple septal pore morphology from fruiting bodies of Jola spp. and cultured isolates of Jola javensis and E. muscicola were consistent with those of related auricularioid phytoparasitic taxa, the rust fungi, and Pachnocybe ferruginea. Jola and Eocronartium can be grown in axenic culture and are not obligate parasites. In nature, the Sporothrix-like anamorph of these fungi may function in dispersal and mating. The previously unknown anamorph of the moss parasites may be instrumental in our understanding of the origin and evolution of the rust uredinial stage.







